Stress management tips
Managing stress is essential for overall well-being and can also have a positive impact on your skin health if you have an inflammatory skin condition, like acne.

Managing stress is essential for overall well-being and can also have a positive impact on your skin health if you have an inflammatory skin condition, like acne.
A recent Dermatology study concluded that most of the information found online regarding diet and acne was misleading or unfounded.
The underlying process is the same in teenage and adult acne, but the pattern of involvement may be different.
There are a number of potential causes for acne and any combination of these may be acting at the same time.
Sleep is increasingly recognised as being key to our general health and wellbeing, with sleep deprivation linked to various skin concerns.
Do you have a teen in your life who is struggling with oily skin, blackheads or breakouts? Read below to discover my tips.
Research indicates that between one and two thirds of female acne sufferers will have a flare around the time of their period.
Back acne – why does it happen and how do we get rid of it? Let’s talk sebum, sweat and skincare products.
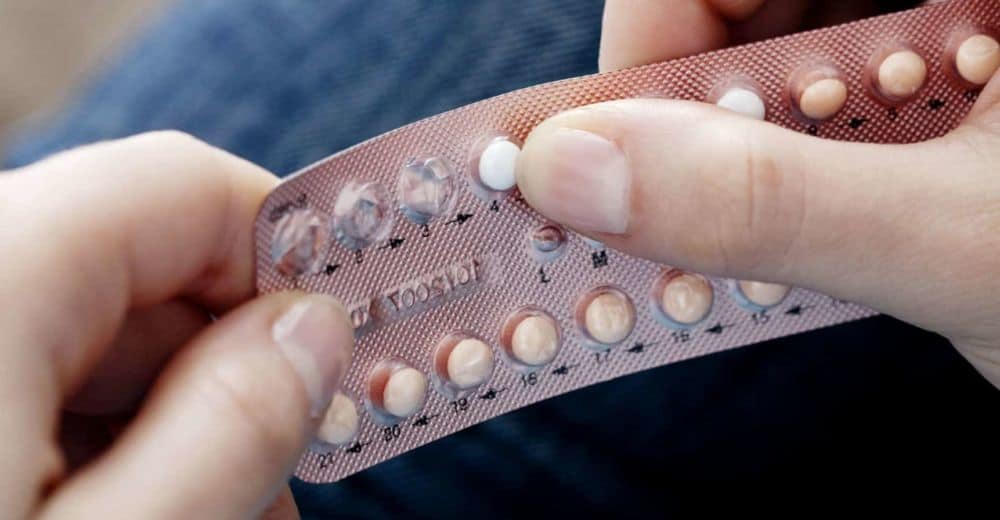
“You know the common story: Woman stops taking pill. Woman experiences acne. But, numerous word-of-mouth experiences aside, why does this happen to so many of us?” This question was recently put to me by Lucy Abbersteen of Marie Claire magazine. Here’s an excerpt of her article: “Pill useage declines steeply with age, from two thirds of women aged between 20 and 24, to just 11% of women in their late 40s,” explains consultant Dermatologist Dr Justine Kluk. “It’s not uncommon for women who have been on the pill for several months or years to notice a flare-up of acne after discontinuation – and the reasons for this are well documented.” “Acne affects 80% of teenagers, making it a very common problem. It also affects 10 to 20% of women over 25, a figure that is definitely on the rise. So this may be a recurrence of acne in those previously affected.” But, hang on – what about if you never experienced acne before the pill? Don’t get too excited. “Acne can also start in adulthood for the first time,” Dr Kluk adds. “In any event, the time of life when acne peaks is similar to the stage at which many women decide to start the contraceptive pill.” “The combined pill is in fact a very effective acne treatment and many women will find that their blemishes improve – or even disappear – as long as they are taking it. The oestrogen component appears to inhibit acne by a variety of mechanisms including reducing production of androgens (responsible for oil production and pore-blocking), and reducing the amount of active free testosterone in the blood.” Unfortunately, because of the individual differences at play and lack of research, it’s not known exactly how many women will see a flare-up or experience a first case of acne upon pill cessation. “The natural history of acne means that a proportion of women who take the pill will ‘grow out’ of their acne while taking the combined pill, and therefore won’t experience a flare-up when they stop taking it. Others, however, will find their acne recurs or appears for the first time once treatment is discontinued; which suggests the pill was masking the acne all along.” Long story short: You may have had acne all along but the pill was masking it, or you had it before and your contraception was acting as an acne treatment. If you are concerned about acne returning when coming off the pill, speak to your GP or see a dermatologist to put a plan of action in place. Dr Kluk adds that it’s worth noting some progesterone-only contraception (the mini pill, depot injection, progesterone coil or implant) can actually be acnegenic. “Use must be discussed carefully with your GP or gynaecologist if you have a history of stubborn acne,” she says. Click here for the full article. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
With sunny weather on the horizon for the upcoming bank holiday, off-the-shoulder tops and strappy dresses mean that it’s time to think about how to finally get rid of back acne or “bacne”. Some of my top pointers are listed below, but you can read my advice in Glamour by clicking here for the full article. 1. Shower every day. 2. Look for a shower gel or body wash containing the ingredients salicylic acid, glycolic acid or lactic acid and use an exfoliating scrub in the shower two or three days a week to prevent dead skin cells from building up and blocking your pores. 3. Apply a moisturiser to soothe and repair your skin barrier, but make sure that any products you leave on your skin are labelled ‘non-comedogenic’, meaning they won’t clog your pores. 4. Shower as soon as possible after exercise. Bacteria loves sweaty skin so it is important to remove your gym clothes as soon as possible, especially bra tops. 5. Wash bras after every wear. 6. Carry a spare T-shirt with you if you tend to sweat more in warmer weather. 7. Whatever you do, don’t pick, squeeze or scratch your spots. This increases inflammation and can lead to scarring. If you’ve tried all of these things and are still struggling to get on top of your breakouts or are aware of developing scars, come see me to discuss the prescription treatments that are available. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Slathering your skin in petroleum jelly before bed is all the rage in Korean beauty circles. But is it any good for your complexion? Jacqueline Kilikita from Stylist magazine investigates. To read my comments on this craze and for some more evidence-based skincare solutions that won’t leave you with a face full of pimples and blackheads, click here. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Whether you’re dealing with blackheads, whiteheads or the cystic, under-the-skin kind, spots can be debilitating to live with. You don’t have to suffer though, because there is effective treatment. I was recently interviewed by Jacqueline Kilikita on behalf of Elle Magazine to help readers decode some of the different acne treatments available. In the spirit of sharing, I thought I’d post the full answers to her questions below as they may be useful to anybody considering treatment for breakouts. Remember, effective control of blemishes is not a one size fits all situation. If a treatment hasn’t worked for someone else you know, it doesn’t mean it won’t work for you – and vice versa. When I am making a treatment plan for a new patient with acne in my clinic, there are a number of factors I take into consideration before prescribing a certain medication. This includes the types of spots you have, where they are on the body, if you are developing scarring or discolouration and what treatments you may already have tried. Sometimes a combination of treatments may be needed if they haven’t worked alone. If you are suffering with acne and would like effective treatment and skincare advice from someone who understands how it feels from personal experience, I’d love to help you. Click on the pink Contact button at the bottom of this blog post to get in touch. Retinoid creams Topical retinoids are derived from vitamin A and work by unclogging pores. They are the treatment of choice for blackheads and closed comedones, the small, stubborn skin-coloured bumps that often appear on the forehead and sides of the cheeks or jawline. Topical retinoids also have direct anti-inflammatory effects and can be combined with other treatments, such as oral antibiotics, for treating more inflamed spots and maintaining results afterwards. Side effects include include redness, dryness, itching and stinging. A good Consultant Dermatologist will give you tips on how to introduce these and which skincare products to combine them with to improve tolerability. Increased sensitivity to the sun means that treatment is usually applied at night and using a non-comedogenic (non pore-blocking) SPF in the morning is strongly recommended. Benzoyl peroxide Benzoyl peroxide works by killing the bacteria that cause acne. It can be applied regularly to help control ongoing breakouts and on an ad hoc basis to reduce flare-ups. The main downside of benzoyl peroxide is that it can cause skin irritation, so you only need to apply a small amount to affected areas or redness and peeling are likely. It can also bleach your towels, clothing and bedsheets so be careful when and how you apply it and consider wearing an old T-shirt to bed if you are applying it to your back or chest. Antibiotic lotions or gels Topical antibiotics, such as erythromycin and clindamycin, are effective acne treatments but should not be used on their own wherever possible due to the risk of developing bacterial resistance. They can, however, be combined with benzoyl peroxide to reduce this risk and to improve results as they tackle bacteria in different ways. Isotretinoin (Roaccutane) Isotretinoin is an oral retinoid and the treatment of choice for severe or persistent acne associated with nodules or cysts, scarring or psychological distress and when other first-line treatments have failed. It works by suppressing sebaceous gland activity, helps us to shed our dead skin cells more effectively to prevent blocked pores and also reduces inflammation and the growth of P. acnes, the bacteria implicated in acne development. Isotretinoin is the most effective anti-acne treatment available, but does have some important side effects and may not be suitable for everyone. These include a high risk of birth defects, meaning that females must take careful steps to prevent pregnancy during treatment and close supervision by a Dermatologist experienced in prescribing the drug is mandatory. Dry, cracked lips are common, blood tests must be done to monitor cholesterol and liver function, alcohol intake should be restricted and prolonged sun exposure must be avoided as there is a higher risk of getting a sunburn. Spironolactone A medicine called spironolactone may also be helpful in some people by reducing the effects of testosterone on the skin. Prescription of this needs to be decided on as case by case basis by a Consultant Dermatologist, however, as it is licensed for the treatment of Polycystic Ovarian Syndrome (PCOS), not acne per se. Spironolactone is often taken alongside the contraceptive pill as it can disrupt your menstrual cycle and it cannot be taken if you are planning a pregnancy due to potential effects on the developing baby. At higher doses, spironolactone is used as a diuretic so needing to pee more frequently is also possible at lower doses. Spironolactone helps control spots in a third of people, reduces them in another third and has no effect on the final third. Light and laser treatments Although limited data has shown that laser or light treatments may improve acne in certain individuals, these are not recommended routinely as there is much less evidence of their benefits compared to prescription therapy when used for the wider population. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
When it comes to finding a wonder treatment for a smoother, softer and more radiant complexion, there’s no shortage in “out there” options. But how far would you go in a bid to improve your skin? And could you actually make things worse for yourself with blackheads and breakouts? Women’s Health investigates slugging, the latest trend to join the crowds and, far from using slugs, all it requires is a household staple – Vaseline. To read my comments in Emma Pritchard’s article, click here © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Blackheads are a mix of oil and dead skin cells sitting in the pores. Exposure to air causes them to oxidise and turn black giving them their characteristic appearance. They start to appear in puberty around the same time that sebum production increases and one of the most common complaints I hear from teenage patients is that they are self conscious about visible pores or blackheads, especially on the nose. Establishing a skincare routine and teaching teens how to look after their skin is important, both for skin health and for self-esteem. I usually suggest the following tips for those who want to try something over the counter before seeing a doctor: 1. Wash your face morning and evening with a mild cleanser, such as Cetaphil Gentle Skin Cleanser. For those with very oily skin, foaming cleansers like Bioderma Sebium Purifying Cleansing Gel or salicylic acid-containing cleansers like Garnier Pure Active Intensive Anti-Blackhead Charcoal Gel Wash and Neutrogena Visibly Clear Spot Clearing Facial Wash can be used in the morning instead. 2. Blackheads and acne are not because you are dirty so scrubbing too hard, or using harsh exfoliators, is not particularly helpful and may actually increase inflammation. 3. Apply a sun protection moisturiser after cleansing in the morning. Acne blemishes can leave dark marks on the skin if not properly protected from the UV rays in sunlight. Choose a broad spectrum product with SPF30 or higher e.g. La Roche-Posay Anthelios or Garnier Ambre Solaire. Always check the label for the words “non-comedogenic” which means the product won’t block the pores. 4. There are some really good products for concealing acne blemishes and improving self-consciousness e.g. Vichy Dermablend Corrector Stick. Mineral make-up containing zinc oxide or titanium dioxide is great for absorbing excess oil and camouflaging redness. I like the range from Bare Minerals. 5. In the evenings, a targeted bacteria-zapping gel like benzoyl peroxide e.g. Acnecide or a pore unblocking agent containing salicylic acid e.g. La Roche-Posay Effaclar Duo can be applied to affected areas after cleansing. 6. Follow with a light moisturiser, such as La Roche-Posay Toleriane Fluide or Effaclar H. Moisturiser makes it easier to tolerate the treatment creams in the previous step which may otherwise cause dryness and peeling. Again, make sure that moisturisers or any other leave-on products are labelled non-comedogenic. 7. Wash your hair regularly and tie it back away from your face. Greasy hair, or application of hair serums and gels, can cause breakouts on the forehead. Wearing a headband or hat should also be avoided if you are prone to spots around your hairline or on your forehead. 8. Remove sweaty clothes as soon as possible after sport or exercise and cleanse your skin thoroughly. If sweat remains on the skin for prolonged periods, acne-causing bacteria will thrive. 9. For boys who are starting to shave, be careful to avoid nicking any existing spots. Clean the blade regularly, make sure it is sharp and shave in the direction of the hair growth. 10. Try to break the habit of touching your face and, whatever you do, do not squeeze or pick your blackheads. This can introduce infection and may also lead to permanent scarring. Instead, try a pore cleansing face mask once or twice per week, such as Garnier Pure Active Intensive 3 in 1 charcoal mask or The Body Shop tea tree skin clearing clay mask. If this doesn’t help, you could have your blackheads professionally extracted by an experienced beauty therapist under strict hygienic conditions every month or two. 11. It might sound obvious, but change your sheets weekly. This is especially important for your pillowcase where grease can build up over time and rub off on your skin as you sleep. 85% of teenagers will experience some form of acne at one time or another and I try to reassure my patients that they are not alone. Nonetheless, it should not be considered a rite of passage that everyone has to go through regardless of the severity. If your teen has lots of red and inflamed bumps, dark marks or signs of scarring, or if their skin is starting to impact their self-esteem, I’d love to be able to help. To book an appointment, call my team on 0203 733 3225. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Adult acne is on the rise. As London’s go-to Consultant Dermatologist for acne and acne scarring, it was a pleasure to be interviewed for Lucy Partington’s awesome feature in this week’s Stylist about the latest breakout breakthroughs. Click here to read about the therapies, foods and products at the heart of research into combatting acne. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
A question that I get asked a lot by patients who have come to see me in the clinic for acne treatment is whether food may be contributing to their breakouts. This is hardly surprising as I can remember being told very clearly when I was a teenager that my spots were caused by eating chocolate. These days, speculation about what we should be eating to lose weight, be healthier and live longer is as hot a topic as ever. With this in mind, I thought it might be useful to put the record straight and share with you what the research shows about diet and acne. In guidelines published by the American Academy of Dermatology (AAD) in 2016 (1), the role of diet in adult and adolescent acne was investigated. To my count, 13 studies were identified by authors after searching the medical literature on the subject. Many of these studies were small in size so it is difficult to draw firm conclusions from them. All is not lost, however, because if multiple small studies show similar effects, it may be possible to identify trends that can be investigated in future to determine if there is a true association. 1. Glycaemic index Glycaemic index is a number. It gives you an idea about how fast your body converts the carbohydrates in a particular food into glucose (sugar). Some foods can make your blood sugar rise very fast. This is because refined sugars and bread, for example, are easier for your body to change into glucose than more slowly digested carbohydrates like vegetables and whole grains. The smaller the number, the lower the glycaemic index and the less impact the food has on your blood sugar. 23 Australian males aged 15-25 were observed over a 12 week period and 32 Koreans aged 20-27 were observed for a 10 week period (2,3). In both studies, subjects who were asked to follow a low glycaemic index diet showed a significant improvement in the severity of their acne at the end of the trial period compared to those who didn’t. Although these 2 studies are the most rigorous to date regarding the effects of glycaemic index on acne, a small number of other studies also supported this association. 2. Dairy Several studies were identified suggesting that dairy products may aggravate acne. 47355 adult women were asked to recall their high-school diet and whether they had been diagnosed with acne by a physician. In this particular study, acne was associated with higher quantities of milk intake, particularly skim milk (4). Because this study relied on memory, there were concerns about it’s accuracy. Further studies performed in a prospective manner have also suggested a link between milk consumption and acne, with the association most marked for skim milk, but the data is still pretty limited. 3. Miscellaneous Some small preliminary studies were found examining the role of antioxidants, probiotics and fish oil on acne, but the AAD comment that the existing evidence is not strong enough to support any recommendations regarding these dietary factors at this time. Bottom line The role of diet in acne remains an area of intense interest and there are still many unanswered questions. We know that acne has a strong genetic component, but it has also been proposed that the rise of adult acne in recent times may be linked to the modern Western diet as well as lifestyle factors, such as stress. Thankfully, further research is underway which will hopefully help us to answer these questions. For now, the American Academy of Dermatology concludes: – Current data is not strong enough to support specific dietary changes in the management of acne. – Emerging data suggests that high glycaemic index diets may be associated with acne. – Limited evidence suggests that some dairy, particularly skim milk, may influence acne. It is therefore important that you discuss these issues very carefully with a doctor knowledgeable about acne before eliminating entire groups of food from your diet as this may lead to nutritional deficiencies that can impact your broader health and wellbeing. A healthy, balanced diet remains the best recommendation at this time. If you are struggling with acne and would like non-judgmental advice and effective treatment, please contact my team to book an appointment as I would love to help. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system. References: 1. Zeingein AL, Pathy AL, Schlosser BJ et al. Guidelines for the management of acne vulgaris. J Am Acad Dermatol 2016. 74(5):945-73.e33. 2. Smith RN, Mann NJ, Braue A et al. The effect of a high-protein, low glycemic-load diet versus a conventional, high glycemic-load diet on biochemical parameters associated with acne vulgaris: a randomized, investigator-masked, controlled trial. J Am Acad Dermatol. 2007;57:247-256. 3. Kwon HH, Yoon JY, Hong JS, Jung JY et al. Clinical and histological effect of a low glycaemic load diet in treatment of acne vulgaris in Korean patients: a randomized, controlled trial. Acta Derm Venereol. 2012;92:241-246. 4. Adebamowo CA, Spiegelman D, Danby FW et al. High school dietary dairy intake and teenage acne. J Am Acad Dermatol. 2005;52:207-214.
Is wearing makeup on an aeroplane actually that bad for your skin? Journalist Jacqueline Kilikita and the team at Refinery29 asked me this very question recently. To see what I had to say on the matter, click on the link below. To be absolutely clear, I am not recommending that you do wear makeup when you fly. My advice is to always stick to your normal skincare routine whenever and wherever practical. So, it’s not a disaster if you wear makeup on a short-haul flight and I wouldn’t have thought that this should be particularly detrimental to your skin health in the bigger picture. You won’t, however, find any Dermatologist who says it’s okay to sleep with your makeup on and, to my mind, the same applies for removing your makeup before you go to sleep on a long-haul flight. If you can’t face the idea of boarding barefaced, opt for non-comedogenic products if your skin is prone to breakouts. Lightweight, hydrating tinted moisturisers or BB creams are your best bet if your skin gets dry when you fly. Happy reading! http://www.refinery29.uk/2018/01/187478/wearing-makeup-plane-skin © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
I get asked all the time about why I decided to become a dermatologist. The short answer is this. Acne. I started to get spots when I was about 12 years old. My dad bought me Clearasil and told me that I would grow out of it. He’d grown out of it when he was my age after all, but not before developing scarring on his cheeks which is still there today in his sixties. So, I used my facewash and sometimes a bit of toothpaste (or Sudocrem or whatever happened to be knocking about on the bathroom shelf for that matter) and patiently waited for it to go away. Having grown up in South Africa, my mum was always very concerned about skin cancer. I remember very clearly, later on as a teenager, being taken to a dermatologist to have a mole on my right shoulder checked. When I sat down on the examination couch the first thing the specialist said to us was “Never mind the mole. What are you doing about her acne?” This was just the start of my lifelong battle with breakouts, and harsh as it sounded back then, I was relieved for the validation that this thing that was a source of real unhappiness to me was deserving of proper attention and that now we were really going to do something about it. This is where my fascination with skin health began and how my passion and determination to help others feel good about their skin started. Acne is the medical term used to describe spots or breakouts. It is easily the most common skin concern there is, affecting as many as 85% of teens. Unfortunately, research shows that more and more of us are continuing to suffer with it in our twenties, thirties and beyond meaning that spots are definitely not just a teenage issue. In fact, it is estimated that up to 20% of adult women are still battling blemishes. When you think that acne can lead to scarring, poor self-image and loss of confidence, this amounts to a big problem. If you’ve suffered with persistent acne, you’ll recognise the feeling that your face never feels clean. No matter how much time or money you spend on grooming, you still feel like a spotty mess. You long to be one of those carefree people who wakes up 5 minutes before they need to leave the house in the morning. Instead, you have to put aside a full 30 minutes to try and painstakingly conceal each and every spot and you definitely need to get to the bathroom first if you have a new partner for fear that they might reject you if they knew what you really looked like. Yes, some people can manage the occasional pimple at home with appropriate store-bought products or advice from a GP. Many others are fed up by a lack of improvement and are understandably worried about developing dark marks or permanent scarring if their symptoms are left unchecked. Emotional scarring should not be downplayed either as acne erodes self-esteem, causing sufferers to feel embarrassed and isolated. It doesn’t have to be like this! If you want really effective treatment for persistent acne or scarring, come see me in the clinic to talk about the options because there is plenty we can do. As well as prescriptions and procedures that really work, I’m keen that you have a skincare plan that helps you maintain the results in the longer run so you’ll want to show your skin off, not hide away. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
When I am planning acne treatment for new patients to the clinic, we have a discussion about the most effective management options based on the severity of their symptoms, what kinds of spots they are getting (e.g. blackheads, pustules, nodules, cysts) and what treatments they’ve already tried. Sometimes oral treatment is most appropriate, sometimes creams or gels (known as topical therapy) are most appropriate and often both are needed together in combination. Topical therapy of acne includes the use of agents that are available over the counter e.g. benzoyl peroxide and salicylic acid or via specialist prescription e.g. antibiotics, azelaic acid and retinoids. So what are topical retinoids? In short, they are vitamin A derivatives. Examples include adapalene (Differin), isotretinoin (Isotrex) and tretinoin. They are possibly the most critical topical therapy for acne because they reduce blockage of the pores (the opening of the hair follicle onto the surface of the skin) and are also anti-inflammatory. As well as enhancing most acne treatment programmes, they can also help with maintaining control after discontinuation of oral therapy. Retinoids are ideal for blackheads and, when used in combination with other agents, for most types of acne. Although they are a very useful tool in the management of acne, the use of topical retinoids may be limited by side effects such as dryness, peeling, redness and irritation. They have also been associated with photosensitivity i.e. causing the skin to be more sensitive to the sun. These side effects can all be much easier to tolerate if the steps below are followed: 1. Use a gentle skin cleanser morning and evening. Apply to a wet face and rinse off with lukewarm water. Do not scrub vigorously. 2. Apply your retinoid cream at night before you go to bed. Do not apply it in the morning as it can make your skin more sensitive to the sun. Take precautions to avoid sunburn by applying a non-comedogenic, broad spectrum SPF50 sun protection moisturiser in the morning before applying your makeup or leaving the house. 3. Introduce it gradually. Start off by applying it twice per week at night. It is normal to have a bit of redness or peeling after a few days. After a couple of weeks, increase application to alternate nights if tolerated. This can subsequently be increased to every night after a further two to four weeks if you are tolerating treatment with minimal or no irritation. 4. If the skin irritation is severe, stop the prescription for a few days until it has settled before attempting to reintroduce it even more gradually. 5. Most people will eventually be able to apply their prescription cream every night without any ongoing discomfort, however some will only ever manage alternate nights or twice per week at the most. Do what you can – some treatment once or twice a week is usually better than none at all. 6. Apply the cream (or gel) in a very thin layer to cover all of the areas that you tend to get the acne, not just onto individual spots. The quantity really doesn’t have to be particularly large as this will just increase irritation. 7. Avoid the area directly around your eyes as the skin is more sensitive. 8. If your skin is dry or irritated, you can apply a moisturiser at night by layering it on top of your retinoid cream. Ideally you should wait 15 minutes or so between these steps to prevent the the retinoid being diluted by your moisturiser. Look for a moisturiser that is labelled non-comedogenic. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
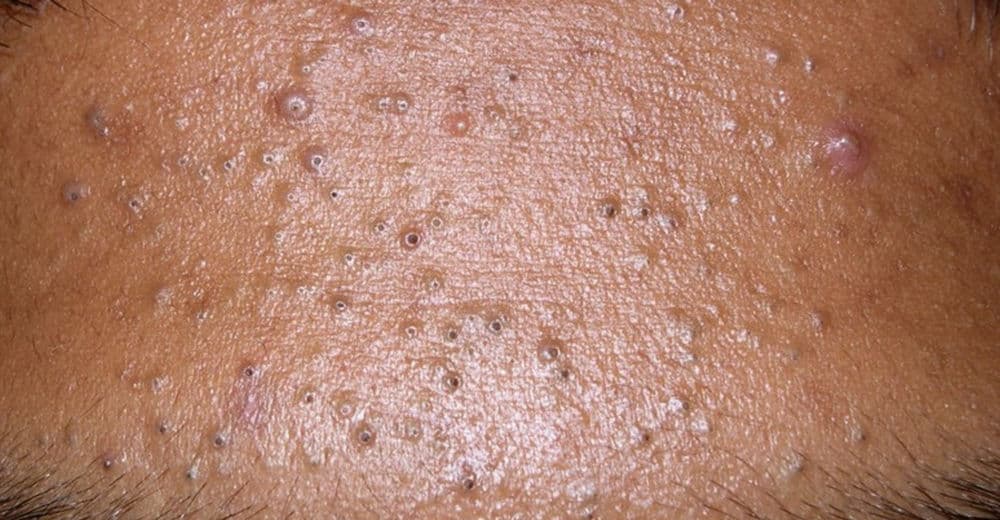
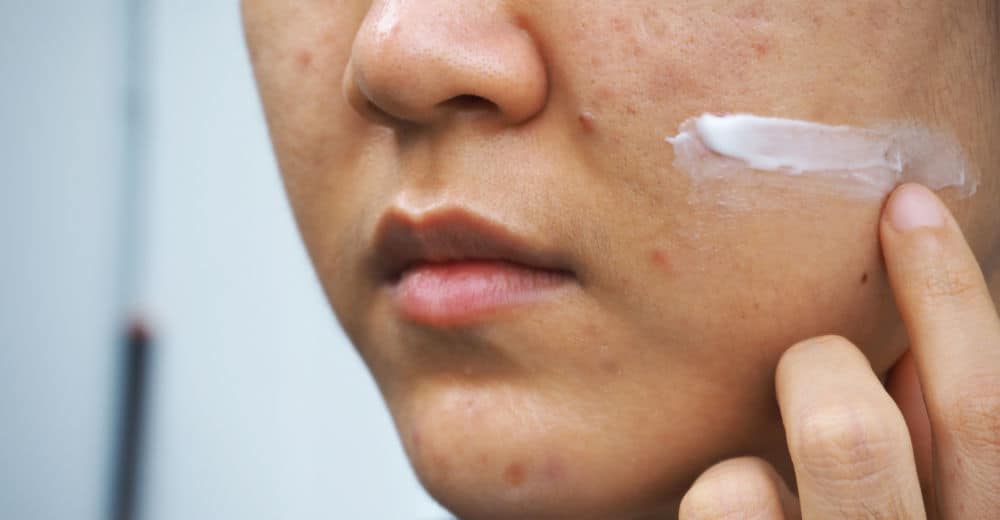
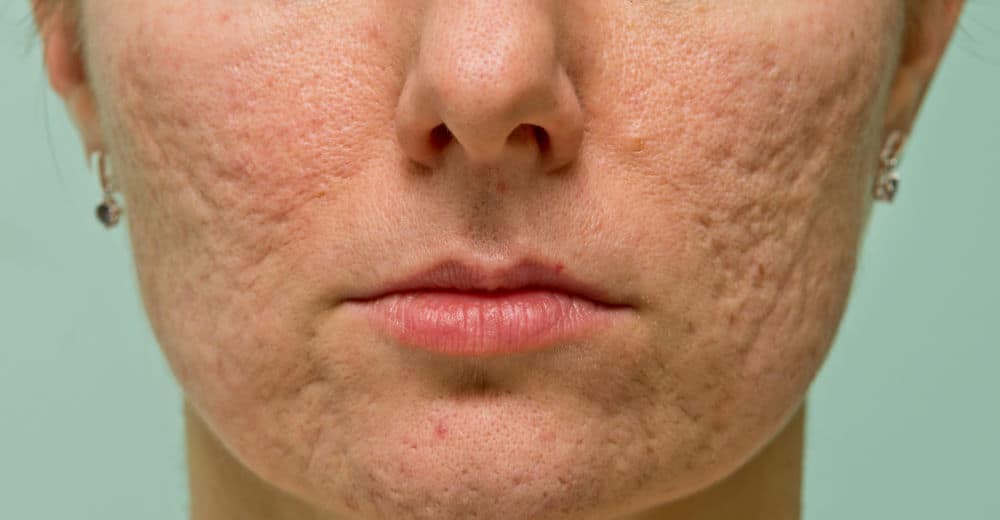
Acne is the medical term used to describe breakouts. For many of us, our first experience of the condition is during puberty when our bodies start to produce higher levels of the hormone testosterone. The sebaceous glands in our skin are very sensitive to even small changes in the level of testosterone and begin to step up production of sebum, the natural oil produced by our skin, as a result. This sebum mixes with dead skin cells and gets trapped in our pores creating an ideal environment for bacteria to thrive. These factors combine to cause inflammation in the skin leading to the development of acne. In its mildest form, acne is responsible for causing occasional spots or pimples. Whilst most of us can manage this at home by using appropriate store-bought products, some people develop a more severe form of the condition that doesn’t go away despite following a good skincare routine. Examples of this include breakouts occurring at multiple sites on the face and body or the appearance of deep, tender nodules and cysts that can lead to permanent scarring if not properly controlled (as shown in the photo above). In these situations, it is important to seek advice from a Dermatologist as prescription treatment is likely to be necessary. Expert help should also be sought if acne is causing loss of self-esteem, anxiety or feelings of embarrassment and social isolation. Whether you are designing a skincare routine at home or following a treatment plan from a Dermatologist, it is essential that the products you use are specifically intended for blemish- prone skin. Key ingredients to look out for include salicylic acid which stops the build up of dead skin cells and zinc, tea tree or witch hazel which are great for soothing inflammation so check for these on product labels. Using the wrong products, or indeed using too many products, can actually make the problem worse. Start by cleansing your face both morning and night. Acne can cause the skin to be red, bumpy and inflamed so a cleanser designed for sensitive skin is a good solution for this. Massage it gently into the skin before rinsing well with lukewarm water and use a soft cloth or flannel to pat dry. I’m not generally a big fan of toners, but for those with greasy skin a toner can be applied next. It is important to recognise that many acne treatments work by reducing oil production and will dry the skin themselves. A gentle tonifying lotion may be tolerated better than ordinary toner in these circumstances as there is less risk of drying the skin out too much. An alternative to this if skin remains greasy is to use pre-prepared pads soaked in glycolic and salicylic acid. The final step in the routine is to use a lightweight moisturiser twice a day to nourish and maintain a healthy skin barrier (unless your skin is exceptionally oily). Looking for the words “non-comedogenic” (meaning non pore-blocking) on the packaging can help guide you to the most appropriate choices. The same goes for sun protection products and makeup which also need to be chosen carefully. I would use a sun protection moisturiser in the morning and a plain moisturiser at night. Finally, grainy scrubs and vigorous rubbing are best avoided in very inflamed acne and squeezing or picking spots is also strongly discouraged as this increases the risk of infection and scarring. Using a clay or charcoal mask once or twice a week is a much better way to draw impurities out of the skin in combination with appropriate acne treatment. If you are following this advice and find that you are not getting the results you need, or if you believe that you are suffering with one of the more severe forms of acne described, please make an appointment to see your GP or Dermatologist for advice. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Spots are probably the most common skin concern of all, affecting as many as 85% of teens at one point or another. Unfortunately, research shows that more and more of us are continuing to suffer with breakouts in our twenties, thirties and beyond meaning that spots are definitely not just a teenage issue. In fact, it is estimated that 10 – 20% of adult women are still battling blemishes. When you think that spots can lead to scarring, poor self-image and loss of confidence, this amounts to a big problem. Before working out how to keep spots at bay, it helps to understand what causes them. There are 3 main reasons that spots occur: Excess sebum production. Sebum is the natural oil produced by our skin. We start making more of it as adolescents which is when spots begin to be a problem for most of us. Build-up of dead skin cells. These dead skin cells mix with the sebum and get trapped in our pores. Bacteria. These bacteria cause inflammation in the skin leading to the angry red bumps and whiteheads that we all dread. In additions to these causes, our genes, diet and lifestyle also play a role in the development of spots. We can’t change our genes, but there are a few lifestyle factors that we can try to address to keep spots at bay. Here are some of my top lifestyle tips for reducing spots: Develop a skincare routine and stick to it every day. It is never too late to start, but it helps to get in the habit from your teenage years onwards. Cleanse your skin well twice daily, follow with a toner to tighten pores and then use a moisturiser designed for spot-prone skin. Using products that aren’t designed for people with breakouts or blemishes can actually make things worse so choose carefully. Consistency is key. Stick to the items in your skincare routine and give them a chance to work. Unless you have a bad reaction to a particular product, I would usually suggest using it regularly for 2 – 3 months before switching if you haven’t noticed an improvement at that point. Don’t fall into the trap of using too many products or chopping and changing every couple of weeks. Similarly, don’t stop using the products when the spots are controlled as you could end up back at square one. Whatever you do, don’t scratch, pick or squeeze. This can introduce bacteria, increased inflammation and may ultimately lead to scarring. Always clean your hands before applying your skincare products and avoid touching your face at other times. Don’t go to bed without removing your makeup. Ideally, you should follow your usual nighttime routine even if it’s late and you’re tired. Keep some cotton pads and a bottle of micellar water next to your bed, however, for those occasions where you may otherwise be tempted to sleep with your makeup on. Greasy hair can contribute to spots on the forehead and around the hairline and neck. If your hair gets greasy easily, keep it tied back off your face and make sure that you wash it regularly. Avoid hats and hair accessories that are likely to trap sweat under your skin and stay away from oily hair serums, gels and waxes that may slide down onto your face blocking your pores. Shower every day. Remove sweaty gym clothes as soon as possible after a workout and don’t delay hopping in the shower. Bacteria thrive in sweaty conditions and can be a particular problem on the back and chest in people who exercise frequently. Change your bedsheets once a week at a minimum. This prevents grease from your pillowcase being rubbed back into your skin. Keep sugary, refined or processed foods to a minimum. This doesn’t mean that you can’t have an occasional chocolate or treat, however. Beyond this, there isn’t a great deal of evidence that cutting particular food groups out of your diet reduces spots. There have, however, been a few small studies suggesting that dairy, especially skimmed milk, may play a role in certain individuals. Always consult with a doctor before cutting anything out of your diet to ensure you are still getting all the nutrients you need. Look after your general health and wellbeing. Lack of sleep and stress can lower your threshold for breaking out. Try to go to sleep at the same time most nights, don’t scrimp on sleep and find ways to let off steam. This may be through doing a hobby, taking a yoga class or relaxing with friends. © 2017 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Breakouts? I’ll be posting my skincare tips for beautiful blemish-free skin this week. No 1: Cleanse your skin morning and evening. Pick a gentle skin cleanser, such as Cetaphil Gentle Cleanser. Wet your face and massage the cleanser into your skin with your fingertips for a minute or so before rinsing and patting dry. No scrubbing, exfoliating, face brushes etc as these simply INCREASE inflammation! This tip is particularly important if you are taking prescription treatment for acne. Many of these prescriptions (e.g. retinoids and benzoyl peroxide) have a drying effect on the skin so an extremely gentle cleanser is of paramount importance in helping you to tolerate your treatment without redness, peeling and irritation. For those with very oily and congested skin, a cleanser containing glycolic or salicylic acid e.g. @SkinCeuticals Blemish + Age cleansing gel may be better suited as these products can help reduce excessive oiliness. No 2: Anyone who has had breakouts has more than likely squeezed a spot before! Although squeezing pimples can make your skin look better in the short term, it can also force the contents even deeper into your skin, increasing inflammation. Squeezing the odd pimple does not always cause scarring, but doing it a lot, and not leaving deeper pimples or nodules alone, almost certainly makes acne worse and increases the likelihood of scarring in the long term. So, bottom line…don’t do it yourself! One option is to have your blackheads professionally squeezed under strict hygienic conditions by a therapist who practices in a dermatology clinic or has been recommended by your dermatologist. Blackheads, or comedones to give them their correct name, are the precursor to all pimples so having these extracted in this way can help control breakouts in combination with the other measures I’ll suggest later on. No 3: My patients often tell me that their breakouts reduce in the sun. There is some truth in this. The sun’s UV rays zap acne-causing bacteria, which is why acne spots may dry up temporarily on sunny holidays. Plus, pimples and red marks look less obvious when your skin is tanned. A few days later, however, redness, bumps and inflammation set in again and you’re back to square one. What’s more, spending too much time in the sun means your blemishes may end up healing with dark scars and spots which can be incredibly difficult to treat or disguise. Beyond acne, UV light also causes free radical damage to the skin, which destroys collagen and elastin, leading to wrinkles. UV rays can also damage the skin’s DNA leading to skin cancer. Acne medication, such as isotretinoin (Roaccutane), tetracyclines and topical retinoids can also make you more sensitive to sunlight, causing your skin to burn faster than it normally would. For all of these reasons, my advice is to stick to your acne skincare routine, and prescription treatment if appropriate, rather than relying on the sun to control your breakouts. Protect your skin from UV rays to prevent permanent scarring and pigmentation. Apply an SPF 30+ broad spectrum (UVA/ UVB) sun protection moisturiser to your face and other exposed sites 365 days a year before you leave the house. These don’t have to be thick and sticky or leave greasy white marks like old-fashioned sunscreens did. Many products now available have the texture of a tinted moisturiser or primer so you can easily layer them under your make-up. Make sure that the label says that the product is non-comedogenic, meaning it won’t clog your pores and increase congestion. My top picks are @janmariniskinresearchPhysical Protectant SPF 30 (tinted), @heliocareuk XF gel SPF 50 (lightly tinted) or 360 gel oil-free SPF 50 (tinted) and @eltamdskincare UV Clear SPF 46 (tinted and plain). Use @garnieruk Ambre Solaire Sensitive Advanced Face Mist SPF50 to top up throughout the day. © 2016 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Retinoid creams are one of the key treatments used by Dermatologists for getting rid of acne. Find out more about these vitamin A-derived prescription treatments in this post http://www.goodzing.com/remedies/dr-justine-kluk/a-guide-to-topical-retinoids-for-treating-acne © 2016 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Without appropriate treatment, dark spots and scars can appear on the skin as acne clears and can be much more of a challenge to manage than the breakouts themselves. Check out my advice on how to prevent and treat acne scarring http://www.goodzing.com/remedies/dr-justine-kluk/how-to-tackle-acne-scarring-and-win © 2016 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
My overview of acne treatment for those stuck with what to do at home and when to see a doctor http://www.goodzing.com/remedies/dr-justine-kluk/an-overview-of-acne-treatment © 2016 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Highlights from my talk to St John’s Wood mum’s group Mums in the Wood about skin changes during pregnancy and how to tackle them http://mumsinthewood.com/nurse-them/specialists/skin-changes-pregnancy-tackle-dr-justine-kluk/ © 2017 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Book an appointment with our Consultant Dermatologists to review your acne history and all the treatment options.
Book now