Does diet play a role in acne?
A recent Dermatology study concluded that most of the information found online regarding diet and acne was misleading or unfounded.

A recent Dermatology study concluded that most of the information found online regarding diet and acne was misleading or unfounded.
The underlying process is the same in teenage and adult acne, but the pattern of involvement may be different.
There are a number of potential causes for acne and any combination of these may be acting at the same time.
Melasma is a common, acquired disorder of hyperpigmentation that causes brown patches on the cheeks, forehead, upper lip and jawline.
Do you have a teen in your life who is struggling with oily skin, blackheads or breakouts? Read below to discover my tips.
Research indicates that between one and two thirds of female acne sufferers will have a flare around the time of their period.
Back acne – why does it happen and how do we get rid of it? Let’s talk sebum, sweat and skincare products.
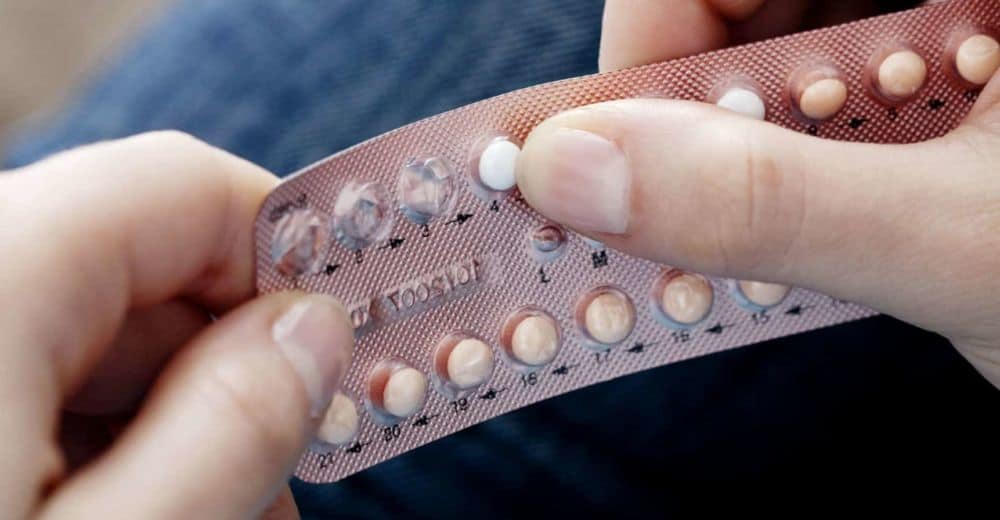
“You know the common story: Woman stops taking pill. Woman experiences acne. But, numerous word-of-mouth experiences aside, why does this happen to so many of us?” This question was recently put to me by Lucy Abbersteen of Marie Claire magazine. Here’s an excerpt of her article: “Pill useage declines steeply with age, from two thirds of women aged between 20 and 24, to just 11% of women in their late 40s,” explains consultant Dermatologist Dr Justine Kluk. “It’s not uncommon for women who have been on the pill for several months or years to notice a flare-up of acne after discontinuation – and the reasons for this are well documented.” “Acne affects 80% of teenagers, making it a very common problem. It also affects 10 to 20% of women over 25, a figure that is definitely on the rise. So this may be a recurrence of acne in those previously affected.” But, hang on – what about if you never experienced acne before the pill? Don’t get too excited. “Acne can also start in adulthood for the first time,” Dr Kluk adds. “In any event, the time of life when acne peaks is similar to the stage at which many women decide to start the contraceptive pill.” “The combined pill is in fact a very effective acne treatment and many women will find that their blemishes improve – or even disappear – as long as they are taking it. The oestrogen component appears to inhibit acne by a variety of mechanisms including reducing production of androgens (responsible for oil production and pore-blocking), and reducing the amount of active free testosterone in the blood.” Unfortunately, because of the individual differences at play and lack of research, it’s not known exactly how many women will see a flare-up or experience a first case of acne upon pill cessation. “The natural history of acne means that a proportion of women who take the pill will ‘grow out’ of their acne while taking the combined pill, and therefore won’t experience a flare-up when they stop taking it. Others, however, will find their acne recurs or appears for the first time once treatment is discontinued; which suggests the pill was masking the acne all along.” Long story short: You may have had acne all along but the pill was masking it, or you had it before and your contraception was acting as an acne treatment. If you are concerned about acne returning when coming off the pill, speak to your GP or see a dermatologist to put a plan of action in place. Dr Kluk adds that it’s worth noting some progesterone-only contraception (the mini pill, depot injection, progesterone coil or implant) can actually be acnegenic. “Use must be discussed carefully with your GP or gynaecologist if you have a history of stubborn acne,” she says. Click here for the full article. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
I was recently featured on the home page of Get The Gloss talking all about my favourite beauty buys with journalist Judy Johnson. In case you missed it, I’ve posted a copy of the original interview just below. For details of where to find the products I’ve mentioned, click on the link at the bottom of this page to go to the article on the Get The Gloss site. Here goes… Where do you prefer to shop for beauty (on or offline) and why? In general, I prefer to shop for new beauty products in-store so I can test how they really look and feel before buying. There is a wonderful pharmacy just round the corner from my clinic on Harley Street (John Bell & Croyden) that carries all of my favourite skincare lines, so this is usually my first port of call. If I’m short on time and already know exactly what I want, or if a product is a bit niche and I don’t have time to trawl around looking for it, I will buy online from escentual.com or skinoracle.com. What’s the last makeup item you bought and why do you like it? I have a bit of a concealer habit and the last makeup item I bought was Bare Minerals SPF20 Correcting Concealer. It has a really nice creamy texture and gives good coverage, so I use it to cover dark circles under my eyes. I love the fact that it doesn’t crease or flake because the skin under my eyes tends to get quite dry as it is. My favourite concealer for covering spots, on the other hand, is the Vichy Dermablend corrector stick. And your most recent skincare purchase? I’m now in my mid 30s, so my top skin priorities are keeping blemishes at bay and also slowing the signs of ageing. This means that I use a product containing vitamin A – a retinoid or retinol – at night. There are a couple I go between, but I’ve just topped up my La Roche Posay Redermic R again. Which products do you gift to friends? I’m pretty strict about sticking to my skincare routine so don’t deviate all that much, even when given new beauty products to try. My sisters and my Mum will often volunteer to “help out” if I’m given something to test and it’s better suited to their skin than mine! In terms of buying gifts for friends, I will often pick a mask or something like that which can be used as a treat. Some of my favourites are the Skinceuticals Phytocorrective masque for soothing tired skin or Medik8 Natural Clay mask for soaking up shine. You have £500 to spend at a makeup counter. Which one do you choose and why? Ooh that’s tough. One of the nicest things about having good skin these days is not having to wear loads of makeup, so I tend to keep things quite simple. If I had £500 to splurge on makeup, I’d probably head to SpaceNK where I usually buy my staple products and add a few extras to the basket. Some of my all-time favourites are Nars – I like their Blush in Orgasm, Bronzing Powder in Laguna and I adore the new limited edition Nars Erdem lipstick in Bloodflower, Laura Mercier – Secret Camouflage Concealer, Eyeko – Brow Gel and Liquid Eyeliner and Hourglass – Liquid Powder Foundation and Veil Translucent Setting Powder. Have you ever had your makeup done at a makeup counter? Which brand and what did you think of it? I was always really self-conscious about my skin as a teenager so the idea of letting someone else do my makeup was terrifying. Once my spots were under control, I could finally enjoy getting glammed up. I had my makeup done at a Nars counter some years ago and was so thrilled with the result that I immediately went and bought all of the products that had been used. Sadly, I wasn’t able to recreate the look when I tried it on my own at home, but there were a few bits that I really loved and still use to this day. The Nars bronzing powder in Laguna is an example. What would be in your Boots or supermarket shopping basket beauty-wise? 1.Aveeno cream and body wash which are both moisturising essentials. 2.Bioderma Atoderm hand cream which I keep by the sink in my clinic and in my handbag. 3.Flexitol balm which I massage into my heels every night after I shower to keep my feet soft and smooth. 4.For my face, I prefer a really mild gel or cream cleanser and a simple, nourishing moisturiser as these help me to tolerate the active ingredients in my skincare routine better. La Roche Posay and Avene have great options. What’s your favourite budget beauty buy? Garnier Micellar Cleansing Water for sensitive skin. It’s super gentle and works just as well as other micellar waters that cost ten times the price. I use it every evening to take off my makeup before cleansing and also carry it in my gym bag so I can make sure my skin is squeaky clean before and after every workout. And the most expensive? Skinceuticals Phloretin CF serum is probably the most expensive skincare product I buy, but well worth the investment. It contains 10% pure vitamin C (L-ascorbic acid) and a host of other antioxidant ingredients which help to reduce damage to the skin from UV rays and city pollution. Unlike lots of other serums, it isn’t greasy and doesn’t clog pores so can be safely used on breakout-prone skin. Where do you get your hair done and what products and treatments/tools do you buy? I absolutely love my hairdresser (Mario Sammour in St John’s Wood) and keep telling him that he’s never allowed to move away or retire as I don’t know what I would do without him. My hair is very fine, but he makes it look like
In case you missed my facial sunscreen recommendation in “9 Facial SPFs Rated By The Experts” in Sheerluxe last week, this is what I had to say… “Having suffered with acne for many years, it’s important for me to use an SPF moisturiser every morning that gives effective UV protection, but won’t give me spots. Garnier Ambre Solaire Anti-Imperfection sun cream is a favourite – it’s non-comedogenic meaning it won’t block pores and contains salicylic acid to soak up shine and target blemishes.” – Dr Justine Kluk, Consultant Dermatologist. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
SPF. Sensible, essential and non-negtotiable. So says journalist Anna Hunter this week in her round up of the new, non-greasy, innovative formulations that are making sunscreen easier than ever to adapt into your daily routine. Keep reading below for my full interview with Get The Gloss about SPF makeup. To see my quotes in the article, including product recommendations, click here. If you want to wear makeup as your sole form of SPF, what should you look out for? I would strongly advise against using makeup as your sole form of SPF. We just don’t apply these products in a thick or even enough layer to get anywhere close to the level of protection provided by a typical sunscreen or sun protection moisturiser. Instead, makeup with SPF should be thought of as your second line of defence against UV rays once you’ve already applied sunscreen because two forms of sun protection are better than one. After cleansing, apply a broad spectrum (UVA/ UVB) sun protection moisturiser with SPF30 or higher to your face, ears, neck and chest. If you’re prone to breakouts, pick a non-comedogenic formulation that won’t clog your pores. Follow with an SPF-containing foundation or powder, depending on how much coverage you’re looking for. If you’re dashing in and out of the office during the day, remember to top up regularly. Would you have to wear a heavy layer or more than you might normally for adequate SPF protection? You would need to apply several times the normal amount of foundation, for example, to get anywhere near the level of protection stated on the bottle. Most of us just don’t want to put that amount of makeup on because it wouldn’t look good. Would you need to reapply SPF makeup throughout the day? Yes. If you’re exposing your skin to the sun, particularly between 11am and 3pm when it’s directly overhead, it is essential to top up your sun protection every couple of hours. Is there a formula that works best in terms of SPF protection (powder, liquid, solid)? Are SPF powders safe? To the best of my knowledge, there haven’t been any head to head studies published in the medical literature comparing the levels of sun protection from different types of foundation. I would therefore choose whichever formula or texture you prefer, provided you have already applied a dedicated sun protection product underneath. The challenge with powders is applying enough to get adequate protection. They are certainly convenient for top-ups, particularly in those who don’t like to wear heavy makeup and may also help soak up sweat that can cause your SPF to wear off, but shouldn’t be relied upon on their own. In terms of safety, skincare products are subject to rigourous scientific testing before becoming commercially available. If there is a concern about the ongoing safety of a particular type of product or research points to new health concerns, they are usually withdrawn pretty quickly. It would seem sensible to stick with reputable brands who specialise in sun protection and have a good track record for safety when selecting your products. Do you have any favourite SPF base makeup that you would recommend? Heliocare oil free compact SPF50 Colorescience Sunforgettable SPF30 or SPF50 Garnier Ambre Solaire nourishing lip protection stick SPF20 In terms of SPF in other makeup, what should you look out for when buying a lipstick/ lip balm/ under eye concealer etc? For lip protection, your best bet is a clear lip balm or stick with the highest SPF that you can find. Most of those currently available are SPF15-20. If you can’t bear the thought of going without lip colour, apply your ordinary lipstick on top of the SPF balm, allowing a few minutes for it to soak in, or use the SPF lip balm as a type of gloss on top. My thoughts about eye shadows, concealers and other types of makeup with SPF are that they aren’t be applied in a thick enough layer to give any meaningful protection on their own so they must always be used as well as sunscreen, not instead of, and simply be considered a boost to whatever protection is already in place. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
I was recently asked in an interview how living in a busy city, like London, can impact the health of our skin. Of course, there are multiple lifestyle and environmental factors to consider, but I think that pollution and stress are worthy of particular mention. If you’d like to know my thoughts on the matter, keep reading below: Can you explain exactly how external factors like pollution, commuting, city air, stress etc contribute to skin damage? We all know that UV rays from sunlight accelerate skin ageing and increase our risk of skin cancer, but city smoke and pollution have also been shown to trigger formation of free radicals in the skin leading to collagen destruction which results in loss of firmness and elasticity, wrinkles and sagging. City air can also leave a layer of dust, grease and grime on the skin which, if not removed effectively when cleansing the skin, can lead to breakouts. You may have noticed this visibly after a busy commute on the underground in rush hour. Stress has been shown to alter the immune functions of the skin and skin barrier function which can lead to increased oil production, pore clogging and growth of the bacteria that predispose us to spots. The bottom line is that city aggressors such as pollution and stress can negatively impact skin health. How much do you think working in a city contributes to the state of our skin? Stress lowers our threshold for getting breakouts. This may be from deadlines looming, working long hours, contending with a difficult commute or not getting enough sleep. Pollution from motor vehicles and factories has been proven to accelerate skin ageing through dark spot and wrinkle formation. A lot of this evidence comes from heavily industrialised areas, such as China. Does avoiding the city centre on the weekend make any difference whatsoever in terms of improving skin health? We know that pollution, smoking and stress can cause skin problems to flare-up and are detrimental to long-term skin health, so it would seem to make sense that being in a cleaner, less polluted environment and getting some respite from our hectic working lives should mean radiant, healthy-looking skin. I’m not sure that a weekend is long enough for this repair and recovery to take place, but it may be a good place to start! Why when we go on holiday does skin tend to improve? People wear less make-up – is that part of the reason? There are a few possible reasons why our skin improves on holiday. Firstly, removing ourselves from the daily grind and actively finding time to relax reduces stress levels which is beneficial for skin health. Many skin problems, including acne, eczema and psoriasis have been shown to improve when we take ourselves out of a stressful environment. Wearing less makeup may lead to an improvement in spots or blackheads if you typically use heavy or long-wearing products to work because you need them to have the staying power to provide coverage from early in the morning till you get home at night. These sorts of products are often occlusive or comedogenic, meaning that they can trigger breakouts. Having a break from them whilst you’re on holiday may give your skin a chance to recover. Finally, gentle sun exposure on holiday can lead to an improvement in certain skin conditions, such as psoriasis, but we are all too aware that lack of UV protection is associated with a higher risk of skin cancer so common sense and the usual sun precautions should still apply. Do you think it is a placebo effect that people think their skin feels better by wearing less makeup at the weekend? I think we would all like the freedom to wear less makeup if we wanted to. In reality, most people with an active skin condition, like acne, don’t feel like they really have any choice because they are embarrassed about how they look and are afraid of being rejected by others. Going make-up free is often seen as the exclusive privilege of those with blemish-free skin, so you can easily understand why we all want to join the club! I try to reassure my patients who are embarking on a course of acne treatment that it is okay to wear makeup if it makes them feel more comfortable, as long as the products are suitable for acne-prone skin. The best bet in this situation is to look for the words “non-comedogenic” on the product label for reassurance that a particular foundation, concealer or powder won’t make breakouts worse. The hope and expectation is that once treatment starts to work, skin confidence increases and the possibility of wearing less makeup becomes a reality. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
I was recently awarded the title FRCP (Fellowship of the Royal College of Physicians) for my work as a Consultant Dermatologist – a huge honour and something I feel very proud of. “But, what exactly is a Consultant Dermatologist?” you might ask. “And what makes you different from from anyone else who gives skincare advice?” I agree that it can be incredibly confusing to work out who is who with all the different terms and titles that get bandied about by medical professionals, like “Dermatologist”, “Cosmetic Dermatologist”, “Aesthetic Doctor” or “Aesthetic Practitioner”. To understand what sets a Consultant Dermatologist apart and why you should see one if you have concerns about your skin, have a read below: 1. What is dermatology Dermatology is the branch of Medicine concerned with health of the skin, hair and nails. Consultant Dermatologists are medical physicians with the highest training and expertise in this field. 2. What training do Consultant Dermatologists receive? In the UK, aspiring Dermatologists start by competing for a highly sought after place at Medical School. This medical degree takes approximately 5-6 years to complete, at the end of which students receive their primary medical qualification and can start to work as a doctor. Following this, they undertake 2 years of general internal medicine training, usually in a hospital setting. During this time, they experience a number of different medical specialties to broaden their knowledge and are expected to take and pass a series of rigorous board examinations known as the MRCP (membership of the Royal College of Physicians). Upon successful completion of this stage, doctors who are hoping to specialise in Dermatology compete again for what is known as a national training number in order to get onto a Dermatology Higher Specialist Training programme. Dermatology is one of the most popular and competitive medical specialties in the UK so only the top few applicants across the country will be accepted. This specialist training takes another 4 years on average and candidates will typically rotate through a number of hospitals to get the widest possible exposure to different skin conditions in this time. At the end of this period, a specialist examination is taken called the Specialty Certificate Examination. If this is achieved and the doctor has also satisfied their trainers that they are safe and competent to practise independently, the doctor will be awarded a Certificate of Completion of Training (CCT) and be entered on the General Medical Council specialist register as a Consultant Dermatologist recognising that they are the only type of doctor with the requisite training and experience to treat patients with skin concerns that can’t be managed by a GP alone. Some Consultant Dermatologists undertake even further qualifications, known as fellowships, if there is a particular field within Dermatology that they wish to sub-specialise in. For example, I was particularly interested in sun damage and skin cancer so I did a year-long fellowship in melanoma. All of this means that most Consultant Dermatologists will have completed about 13-15 years of medical training before they earn the qualification, meaning they are the safest and most knowledgeable doctor to treat your skin concern. 3. Why should someone go see a Consultant Dermatologist? Anyone who has a problem or concern about their skin can benefit from the advice of a Consultant Dermatologist. Examples of reasons to see a Dermatologist include inflammatory skin conditions like acne, rosacea, eczema or psoriasis, mole checks, skin cancer diagnosis and treatment to name a few. In the UK, you can see your NHS GP for advice first and they may refer you to an NHS Dermatology Department if they deem it appropriate or necessary. Appointments can alternatively be booked directly with the office of a Consultant Dermatologist for anybody who wishes to go privately. It is important to remember that cosmetic skin concerns cannot be treated on the NHS. 4. How do you pick the right Dermatologist for you? If you are being referred to an NHS Dermatology department, you may not have a choice as to which particular doctor you see, however they will either be a Consultant Dermatologist themselves or be under the supervision of one. In the private sector, there are lots of healthcare practitioners claiming to be skin experts so it’s important to do your research before booking an appointment. Firstly, check the General Medical Council (GMC) list of registered medical practitioners to confirm that the doctor is on the specialist register so that you can be assured of their training credentials. The list can be accessed here. Next, ask friends and family (or your GP) if they have someone they can recommend from personal experience as this is a good way of filtering the options. Finally, take a look at the doctor’s website or biography to see if they have particular expertise in your condition and might be a good fit for you. For example, in the past few years my practice has focused predominantly on the treatment of acne and acne scarring so I am considered to have particular clinical expertise in this area, something that you will probably have noticed if you’ve read my blogs or looked at my website. If you are struggling with a skin problem, like acne, and would like effective treatment from someone who knows how it feels to suffer with spots first hand, I’d be delighted to help. Please phone my team on 02037333225 to book an appointment to come and see me. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
I’m so thrilled to have been included in Stylist Magazine’s 7 Skincare Experts You Should Be Following On Instagram this week. This is what beauty journalist Elizabeth Bennett had to say about me: Dr Justine Kluk Best for: Targeted solutions for acne and rosacea Thanks to her extensive experience treating patients suffering from acne and rosacea both in the NHS and her private practice, Dr Justine Kluk is a mine of information on the subject. Her feed is a mix of expert product recommendations, her take on beauty trends (the good and the bad), and an insight into what a dermatologist actually uses on her skin. If you don’t already follow me on Instagram, click here to see what all the fuss is about! © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
It seems that summer is here to stay with weather forecasts promising another hot and sunny week! For practical advice about how to protect your skin in the sun, have a read of my tips below: 1. It is always important to protect exposed skin from UV rays to reduce the risk of skin cancer and to prevent premature ageing, pigmentation and exacerbation of skin conditions like rosacea. This is most crucial between April and September in the UK when UV levels are at their peak, but common sense should also apply at other times of year when UV levels are reduced, but not totally absent. 2. Apply a broad spectrum (UVA and UVB) sunscreen with an SPF of 30 or higher to exposed skin 15 minutes before heading outdoors. Look for a non-comedogenic product if you are prone to blackheads or breakouts, meaning that it won’t clog your pores. 3. No SPF offers 100% protection, but the higher the factor the better. For example SPF 15 gives approximately 93% protection compared with 97% for SPF30 and 98% for SPF50. 4. To get the level of protection on the product label, you need to apply the product liberally and in an even layer. As a rule of thumb, a golf ball-sized blob is about the right amount to protect your whole body and a quarter of a teaspoon is about the right amount for your face! 5. Most SPF products will have an expiry date stamped on the packaging or details of when the product should be replaced. In general, sunscreen should be replaced within a year of opening, but mists or sprays may last longer as they are stored in pressurised containers. 6. The terms “mineral” and “physical” sunscreen are often used interchangeably to describe sun protection products that scatter or reflect UV radiation. The primary ingredients in these products are titanium dioxide or zinc oxide. Chemical sunscreens absorb UV radiation and are composed of synthetically-prepared organic chemicals that can be classified as UVA or UVB absorbers. They are often combined with physical sunscreens or with each other to prevent UV radiation from penetrating the epidermis, the skin’s uppermost layer. 7. I would strongly advise against using makeup as your sole form of SPF. We just don’t apply these products in a thick or even enough layer to get anywhere close to the level of protection provided by a typical sunscreen or sun protection moisturiser. Instead, makeup with SPF should be thought of as your second line of defence against UV rays once you’ve already applied sunscreen because two forms of sun protection are better than one. 8. Sweating, swimming and towelling off can reduce the effectiveness of your sunscreen, so it needs to be topped up every couple of hours and as soon as you get out of the pool. Even if you’re just dashing in and out of the office for lunch or on the way home, your sunscreen will lose effectiveness over the course of the day and is likely to have rubbed off a little so care should still be taken with topping up in a city environment. 9. Take extra precautions or head indoors between 11am and 3pm when the sun is directly overhead. Remember that no sunscreen gives 100% protection, so sun avoidance, protective clothing, sunglasses and hats should also be considered. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
What is rosacea? Rosacea is a long term skin condition associated with facial redness and flushing. Although more than 5% of the population are affected, it is frequently misdiagnosed and under-treated as a result. It often appears in the thirties and is more prevalent in those with fair skin. There are a number of factors believed to contribute to the development of rosacea. These include genetics, blood vessel abnormalities, hormonal influences, microorganisms and diet. How might it affect me? Rosacea is so much more than just a red face. It often begins with a tendency to flush or blush more easily. With time, sufferers may develop permanent redness of the nose and cheeks along with a multitude of other unpleasant symptoms, such as pimples, skin dryness and scaling, burning and stinging, and sensitivity to multiple skin care products. Broadly speaking there are four different types of rosacea, but it is not uncommon for these to overlap in the same person. Erythemato-telangiectatic: Redness, flushing and dilated blood vessels. Papulopustular: Acne-like breakouts. Phymatous: Skin swelling and thickening e.g. of the nose (rhinophyma). Ocular: Gritty eyes and swollen lids. As rosacea is such a visible condition, people often describe feeling anxious or embarrassed about their appearance. This may lead to withdrawal from social situations, relationship issues and loss of self-esteem in the workplace. Some may even be too embarrassed to ask for help, or may have been turned away when seeking advice through the usual routes as the psychological impact is often underestimated. What are the treatments? At present there is no cure for rosacea, however there are a number of effective options that can help bring symptoms under control. The choice of treatment depends on the type of rosacea and, of course, patient preference. If flushing is your most troublesome symptom, oral medications otherwise used for anxiety or menopausal flushing e.g. beta-blockers or clonidine, may be recommended. Avoiding triggers is also crucial for this type of rosacea and self-help advice about this is given below. Redness and pimples may be reduced by creams or gels containing antibiotics or azelaic acid. Ivermectin cream is a newer addition to the range of topical agents for rosacea, as is brimonidine gel which improves redness by causing constriction of dilated blood vessels. If these measures do not provide sufficient relief, visible vessels can be targeted very effectively with vascular lasers. For more severe cases of rosacea, a course of oral antibiotics may be recommended to reduce breakouts, swelling and inflammation. Courses may be repeated from time to time for recurrent flares and control can be maintained with topical prescriptions in between times. A dermatologist-only medication, known as isotretinoin, may sometimes be prescribed for stubborn cases although this is an off-license use. When thickening of the skin occurs, Dermatologists or Plastic Surgeons may recommend a surgical procedure to remove excess tissue and create a more natural-looking shape. Is there anything I can do? Absolutely. The following self-help tips may help to reduce rosacea symptoms. 1. Identify and avoid triggers, such as: – exposure to sunlight – strong winds – stress – strenuous exercise – caffeine – alcohol – spicy food 2. Beware of false or inflated promises about skin care products and get testers or samples to try at home before committing to bulk purchases. 3. Keep it simple. Use a gentle cream or gel cleanser for washing your face. Massage it gently into your skin morning and night and rinse off with lukewarm water or wipe off with soft cotton pads if warm water makes you flush. 4. Find a broad spectrum SPF 50 sun-protection moisturiser and apply it every morning, 365 days a year. UV is one of the most common reasons for rosacea to flare, even in cloudy weather. 5. Apply a soothing anti-redness moisturiser before bed. 6. There are some excellent foundations and concealers that neutralise the redness of rosacea and can really boost skin confidence. Creams with a green pigment are particularly helpful. Charities such as Changing Faces in the United Kingdom can also provide advice on skin camouflage and put you in touch with others who are similarly affected. If you are struggling with symptoms like these and would like non-judgmental advice and reliable, effective treatment, come see me in the clinic to talk through the options. Call us on 02037333225 to book your appointment. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Whether you’re dealing with blackheads, whiteheads or the cystic, under-the-skin kind, spots can be debilitating to live with. You don’t have to suffer though, because there is effective treatment. I was recently interviewed by Jacqueline Kilikita on behalf of Elle Magazine to help readers decode some of the different acne treatments available. In the spirit of sharing, I thought I’d post the full answers to her questions below as they may be useful to anybody considering treatment for breakouts. Remember, effective control of blemishes is not a one size fits all situation. If a treatment hasn’t worked for someone else you know, it doesn’t mean it won’t work for you – and vice versa. When I am making a treatment plan for a new patient with acne in my clinic, there are a number of factors I take into consideration before prescribing a certain medication. This includes the types of spots you have, where they are on the body, if you are developing scarring or discolouration and what treatments you may already have tried. Sometimes a combination of treatments may be needed if they haven’t worked alone. If you are suffering with acne and would like effective treatment and skincare advice from someone who understands how it feels from personal experience, I’d love to help you. Click on the pink Contact button at the bottom of this blog post to get in touch. Retinoid creams Topical retinoids are derived from vitamin A and work by unclogging pores. They are the treatment of choice for blackheads and closed comedones, the small, stubborn skin-coloured bumps that often appear on the forehead and sides of the cheeks or jawline. Topical retinoids also have direct anti-inflammatory effects and can be combined with other treatments, such as oral antibiotics, for treating more inflamed spots and maintaining results afterwards. Side effects include include redness, dryness, itching and stinging. A good Consultant Dermatologist will give you tips on how to introduce these and which skincare products to combine them with to improve tolerability. Increased sensitivity to the sun means that treatment is usually applied at night and using a non-comedogenic (non pore-blocking) SPF in the morning is strongly recommended. Benzoyl peroxide Benzoyl peroxide works by killing the bacteria that cause acne. It can be applied regularly to help control ongoing breakouts and on an ad hoc basis to reduce flare-ups. The main downside of benzoyl peroxide is that it can cause skin irritation, so you only need to apply a small amount to affected areas or redness and peeling are likely. It can also bleach your towels, clothing and bedsheets so be careful when and how you apply it and consider wearing an old T-shirt to bed if you are applying it to your back or chest. Antibiotic lotions or gels Topical antibiotics, such as erythromycin and clindamycin, are effective acne treatments but should not be used on their own wherever possible due to the risk of developing bacterial resistance. They can, however, be combined with benzoyl peroxide to reduce this risk and to improve results as they tackle bacteria in different ways. Isotretinoin (Roaccutane) Isotretinoin is an oral retinoid and the treatment of choice for severe or persistent acne associated with nodules or cysts, scarring or psychological distress and when other first-line treatments have failed. It works by suppressing sebaceous gland activity, helps us to shed our dead skin cells more effectively to prevent blocked pores and also reduces inflammation and the growth of P. acnes, the bacteria implicated in acne development. Isotretinoin is the most effective anti-acne treatment available, but does have some important side effects and may not be suitable for everyone. These include a high risk of birth defects, meaning that females must take careful steps to prevent pregnancy during treatment and close supervision by a Dermatologist experienced in prescribing the drug is mandatory. Dry, cracked lips are common, blood tests must be done to monitor cholesterol and liver function, alcohol intake should be restricted and prolonged sun exposure must be avoided as there is a higher risk of getting a sunburn. Spironolactone A medicine called spironolactone may also be helpful in some people by reducing the effects of testosterone on the skin. Prescription of this needs to be decided on as case by case basis by a Consultant Dermatologist, however, as it is licensed for the treatment of Polycystic Ovarian Syndrome (PCOS), not acne per se. Spironolactone is often taken alongside the contraceptive pill as it can disrupt your menstrual cycle and it cannot be taken if you are planning a pregnancy due to potential effects on the developing baby. At higher doses, spironolactone is used as a diuretic so needing to pee more frequently is also possible at lower doses. Spironolactone helps control spots in a third of people, reduces them in another third and has no effect on the final third. Light and laser treatments Although limited data has shown that laser or light treatments may improve acne in certain individuals, these are not recommended routinely as there is much less evidence of their benefits compared to prescription therapy when used for the wider population. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
This month, I’m featured on the Skin Clinic page of Women’s Health sharing a bit about me, my typical day and some of the products I use personally to help keep my own blemishes at bay as London’s go-to acne and acne scarring expert. Read all the juicy details in the full interview below. Enjoy! 1. Name – Dr Justine Kluk 2. Age – 35 (I’ve actually turned 36 since these questions were answered!) 3. Profession – Consultant Dermatologist 4. Typical day I get up early as I like to fit in some exercise before heading to my clinic. I spin three mornings a week at a local studio called Spinnoff near my home in Hampstead. The class is pretty gruelling, but the music is invigorating and I always feel ready to face whatever the day has to throw at me afterwards. Once I’ve showered and changed, I grab a coffee and make my way to my private dermatology clinic in London’s Harley Street. There is no average day in the clinic! Every patient has their own unique story and my job is to ensure that I tailor the treatment and the skincare advice I give to their individual concerns in order to get the best results. Having said this, many patients who come to see me are looking for help with acne and acne scarring. These are my particular areas of expertise, and having suffered personally with persistent breakouts throughout most of my teens and twenties, they know they will find a sympathetic ear and someone who is really motivated to make things better for them from first-hand experience. After clinic, I might meet a friend or colleague for a drink nearby or spend a little time browsing the stores around Oxford Street. I always find myself drawn to the beautiful row of boutiques in St Christopher’s Place, just behind Selfridges, for a bit of window shopping. This is one of the real perks of working in central London as there is so much to do and see and I try my best to take full advantage of it all! 5. Skincare philosophy Keep it simple. Choose products with ingredients you recognise and know to be effective. Give new products time to work – don’t keep chopping and changing. Make sure that the products you pick are suited to your skin type. One size does not fit all. 6. Skincare non-negotiable SPF. It’s a no-brainer! As well as protecting you from skin cancer, wearing a sun protection moisturiser every morning, come rain or come shine, reduces your risk of dark spots, saggy skin, fine lines and wrinkles. There are lots and lots of really nice, cosmetically acceptable sunscreens available these days that don’t leave thick, sticky, white marks everywhere. If you look for the words “non comedogenic” on the package label, they shouldn’t clog your pores either. 7. Personal skincare concern Spots. I suffered with acne from the age of 12 or 13. Like many parents, mine thought I’d grow out of it by the time I reached my twenties. I didn’t and it made me feel totally miserable. It may sound dramatic, but when I did eventually get effective treatment, it was an absolute game-changer and this is the main reason I went to medical school and specialised in Dermatology. I wanted to make sure that no-one else had to feel the way I did when there is treatment that actually works. These days I get to help others with a similar story to me every day and it is so rewarding, both personally and professionally. 8. 3 products you use in the morning and why? In the morning, I splash some lukewarm water on my face then massage a gentle cleanser like La Roche Posay Effaclar H cleansing cream over my skin before rinsing and patting dry. This removes any grease or dirt and prepares my skin for the rest of my routine. Next up is my antioxidant serum. I love Skinceuticals Phloretin CF serum which contains 10% vitamin C. Antioxidants protect your skin from environmental damage like UV rays and city pollution by neutralising free radicals so are great as part of any anti-ageing skincare routine or if your goal is a brighter complexion. Finally, I apply a sun protection moisturiser. Because of my history of breakouts, I will only use a non-comedogenic product and I can highly recommend Garnier Ambre Solaire Sensitive Advanced anti-imperfection sun cream which also contains salicylic acid to help control blemishes. 9. 3 products you use in the evening and why? At night, I use micellar water to remove my makeup before cleansing. I also keep a bottle next to my bed along with some cotton pads in case I am ever tempted to skip my evening routine because I’ve had a late night. Garnier’s new oil-infused cornflower micellar water is a godsend for removing eye-makeup. I follow this with a retinol cream, such as Redermic R by La Roche Posay 3 nights per week. This helps with evening skin tone, preventing fine lines and tightening pores. If my spots have been problematic, I may use a prescription cream at this point instead. Finally, my skin has a tendency to get irritated if I overdo the retinol, particularly in autumn and winter when the air is much drier. I finish my evening routine by applying a soothing moisturiser such as Bioderma Sensibio Rich. By reinforcing the skin barrier, it helps reduce those tight, uncomfortable sensations and also calms redness. If you’re struggling with spots and would like me to help you get them under control, call my team to book an appointment on 02037333225. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of
I get asked all the time about why I decided to become a dermatologist. The short answer is this. Acne. I started to get spots when I was about 12 years old. My dad bought me Clearasil and told me that I would grow out of it. He’d grown out of it when he was my age after all, but not before developing scarring on his cheeks which is still there today in his sixties. So, I used my facewash and sometimes a bit of toothpaste (or Sudocrem or whatever happened to be knocking about on the bathroom shelf for that matter) and patiently waited for it to go away. Having grown up in South Africa, my mum was always very concerned about skin cancer. I remember very clearly, later on as a teenager, being taken to a dermatologist to have a mole on my right shoulder checked. When I sat down on the examination couch the first thing the specialist said to us was “Never mind the mole. What are you doing about her acne?” This was just the start of my lifelong battle with breakouts, and harsh as it sounded back then, I was relieved for the validation that this thing that was a source of real unhappiness to me was deserving of proper attention and that now we were really going to do something about it. This is where my fascination with skin health began and how my passion and determination to help others feel good about their skin started. Acne is the medical term used to describe spots or breakouts. It is easily the most common skin concern there is, affecting as many as 85% of teens. Unfortunately, research shows that more and more of us are continuing to suffer with it in our twenties, thirties and beyond meaning that spots are definitely not just a teenage issue. In fact, it is estimated that up to 20% of adult women are still battling blemishes. When you think that acne can lead to scarring, poor self-image and loss of confidence, this amounts to a big problem. If you’ve suffered with persistent acne, you’ll recognise the feeling that your face never feels clean. No matter how much time or money you spend on grooming, you still feel like a spotty mess. You long to be one of those carefree people who wakes up 5 minutes before they need to leave the house in the morning. Instead, you have to put aside a full 30 minutes to try and painstakingly conceal each and every spot and you definitely need to get to the bathroom first if you have a new partner for fear that they might reject you if they knew what you really looked like. Yes, some people can manage the occasional pimple at home with appropriate store-bought products or advice from a GP. Many others are fed up by a lack of improvement and are understandably worried about developing dark marks or permanent scarring if their symptoms are left unchecked. Emotional scarring should not be downplayed either as acne erodes self-esteem, causing sufferers to feel embarrassed and isolated. It doesn’t have to be like this! If you want really effective treatment for persistent acne or scarring, come see me in the clinic to talk about the options because there is plenty we can do. As well as prescriptions and procedures that really work, I’m keen that you have a skincare plan that helps you maintain the results in the longer run so you’ll want to show your skin off, not hide away. © 2018 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
My overview of acne treatment for those stuck with what to do at home and when to see a doctor http://www.goodzing.com/remedies/dr-justine-kluk/an-overview-of-acne-treatment © 2016 Dr Justine Kluk. Any redistribution or reproduction of part or all of the contents of this post in any form is prohibited. You may not, except with our express written permission, copy, distribute or commercially exploit the content. Nor may you transmit it or store it in any other website or other form of electronic retrieval system.
Book an appointment with our Consultant Dermatologists to review your acne history and all the treatment options.
Book now